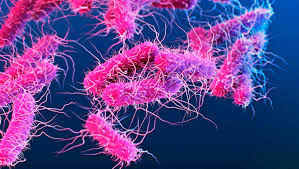
Drug-resistant Shigella, often referred to as “superbug diarrhea,” is an emerging global health concern that is gaining attention due to its increasing resistance to commonly used antibiotics. Shigellosis This infection is caused by Shigella bacteria and primarily affects the digestive system, leading to severe diarrhea and other gastrointestinal complications. What makes this condition particularly alarming is its ability to resist standard treatments, making infections harder to control and manage.
In recent years, health authorities including the World Health Organization have raised concerns about the rapid spread of antibiotic-resistant bacteria, including drug-resistant Shigella. This has turned a once treatable illness into a more serious public health issue, especially in areas with limited healthcare resources and poor sanitation.
What is Drug-Resistant Shigella?
Drug-resistant Shigella is a form of bacterial infection where the Shigella bacteria have developed resistance to antibiotics that were previously effective in treating the illness. This condition falls under the broader category of antimicrobial resistance (AMR), which occurs when microorganisms evolve to survive exposure to medications designed to kill them.
Shigella infections, also known as shigellosis, are highly contagious and spread easily in crowded environments. The drug-resistant form of this infection is more difficult to treat and can lead to prolonged illness, increased risk of complications, and higher chances of spreading the infection to others.
How Does Shigella Spread?
The spread of Shigella bacteria primarily occurs through the fecal-oral route, meaning that the bacteria are transmitted when contaminated material enters the mouth. This can happen in several ways, often linked to poor hygiene practices and unsafe food or water.
One of the most common transmission routes is through direct contact with an infected person, especially in environments such as households, daycare centers, and schools. Even a small amount of bacteria can cause infection, making it extremely easy to spread. Contaminated food and drinking water are also major sources, particularly in areas where sanitation systems are inadequate. In some cases, the bacteria can spread through touching contaminated surfaces and then touching the mouth without proper handwashing.
Symptoms of Drug-Resistant Shigella:
The symptoms of drug-resistant Shigella are similar to those of regular shigellosis but may be more severe and longer-lasting due to limited treatment options. Symptoms typically appear within one to three days after exposure to the bacteria.
The most common symptom is diarrhea, which may range from mild to severe. In many cases, the diarrhea becomes bloody, indicating damage to the intestinal lining. Patients often experience abdominal cramps and pain, which can be intense and persistent. Fever is another common symptom, reflecting the body’s response to infection. Nausea and vomiting may also occur, along with a general feeling of weakness and dehydration.
Because the bacteria attack the intestinal tract, frequent and urgent bowel movements are common, sometimes accompanied by a feeling of incomplete emptying. In severe cases, especially among children and elderly individuals, dehydration can become life-threatening if not treated promptly.
Causes of Drug-Resistant Shigella:
The primary cause of this infection is exposure to Shigella bacteria that have developed resistance to antibiotics. This resistance occurs over time due to the misuse and overuse of antibiotics in both humans and animals. When antibiotics are used unnecessarily or incorrectly, bacteria can adapt and become stronger, eventually rendering these medications ineffective.
Poor sanitation and hygiene practices significantly contribute to the spread of drug-resistant Shigella. In regions where clean water and proper waste disposal systems are lacking, the bacteria can easily contaminate food and water supplies. Close living conditions, such as crowded urban areas or refugee camps, also increase the risk of transmission.
Travel to regions experiencing outbreaks can expose individuals to drug-resistant strains, especially if they consume contaminated food or water. Additionally, inadequate infection control in healthcare settings can contribute to the spread of resistant bacteria.
Diagnosis of Shigella Infection:
Diagnosing drug-resistant Shigella involves identifying the presence of Shigella bacteria in a patient’s stool sample. Laboratory testing plays a crucial role in confirming the infection and determining whether the bacteria are resistant to antibiotics.
Stool culture is the most common method used to detect the bacteria. Once identified, further testing is conducted to assess antibiotic sensitivity, which helps doctors choose the most effective treatment. In some cases, additional tests may be required to rule out other causes of diarrhea and gastrointestinal symptoms.
Early diagnosis is essential for managing the infection and preventing its spread, especially in communities where outbreaks can occur rapidly.
Treatment of Drug-Resistant Shigella:
Treating drug-resistant Shigella can be challenging due to limited effective antibiotics. While mild cases may resolve on their own without the need for antibiotics, more severe infections require careful medical management.
The primary focus of treatment is supportive care, which includes maintaining hydration and electrolyte balance. Patients are advised to drink plenty of fluids, including oral rehydration solutions, to prevent dehydration. In severe cases, intravenous fluids may be necessary.
When antibiotics are required, doctors must rely on laboratory testing to select medications that are still effective against the resistant strain. This process can delay treatment and increase the complexity of care. Improper use of antibiotics should be avoided, as it can worsen resistance and make future infections harder to treat.
Rest and proper nutrition also play an important role in recovery, helping the body fight off the infection more effectively.
Prevention of Drug-Resistant Shigella:
Preventing the spread of drug-resistant Shigella requires a combination of personal hygiene practices and public health measures. Good hand hygiene is one of the most effective ways to reduce the risk of infection. Washing hands thoroughly with soap and clean water, especially after using the toilet and before handling food, is essential.
Safe food handling practices are equally important. This includes cooking food thoroughly, avoiding raw or undercooked items, and ensuring that drinking water is clean and safe. In areas where water quality is uncertain, boiling or filtering water can help prevent contamination.
Avoiding close contact with infected individuals and maintaining cleanliness in shared environments can further reduce the spread. Public health efforts, such as improving sanitation systems and promoting awareness about antibiotic resistance, are crucial in controlling outbreaks.
Responsible use of antibiotics is another key preventive measure. Antibiotics should only be used when prescribed by a healthcare professional and should be taken exactly as directed. This helps prevent the development of resistant bacteria and preserves the effectiveness of existing treatments.
Why is Drug-Resistant Shigella a Global Concern?
Drug-resistant Shigella is considered a global health threat because it represents a growing challenge in the fight against infectious diseases. As bacteria become resistant to antibiotics, the options for treatment become limited, leading to longer illness durations, higher healthcare costs, and increased risk of complications.
The ease with which Shigella spreads, combined with its low infectious dose, makes it particularly difficult to control. In a highly connected world, outbreaks can quickly spread across borders through travel and trade. This highlights the need for coordinated international efforts to monitor and manage antibiotic resistance.
Possible Complications:
If left untreated or poorly managed, drug-resistant Shigella can lead to several complications. Severe dehydration is one of the most immediate risks, especially in young children and older adults. Persistent diarrhea can cause significant fluid loss, leading to weakness and, in extreme cases, organ failure.
Other complications may include intestinal damage, bloodstream infections, and a condition known as reactive arthritis, which can cause joint pain and inflammation. In rare cases, neurological complications such as seizures may occur, particularly in children.
Who is at Higher Risk?
Certain groups are more vulnerable to drug-resistant Shigella infections. Children, especially those under five years of age, are at higher risk due to their developing immune systems and increased exposure in daycare settings. Elderly individuals are also more susceptible, particularly if they have underlying health conditions.
People with weakened immune systems, such as those undergoing medical treatments or living with chronic illnesses, are at greater risk of severe infections. Travelers visiting areas with poor sanitation may also be exposed to drug-resistant strains.
Frequently Asked Questions:
Many people wonder whether drug-resistant Shigella is life-threatening. While most cases can be managed with proper care, severe infections can lead to serious complications if not treated promptly. Another common question is whether the infection can be prevented entirely; while it may not be possible to eliminate the risk completely, good hygiene and safe practices significantly reduce the chances of infection.
People also ask whether antibiotics should always be used. The answer depends on the severity of the infection and laboratory results, as unnecessary use of antibiotics can worsen resistance.
Conclusion:
Drug-resistant Shigella represents a growing challenge in modern healthcare, highlighting the urgent need for awareness, prevention, and responsible antibiotic use. As a highly contagious infection with increasing resistance to treatment, it poses a serious threat to global health. However, with proper hygiene practices, early diagnosis, and careful medical management, its impact can be reduced.
Understanding the symptoms, causes, and preventive measures is essential for protecting individuals and communities. By staying informed and adopting healthy practices, we can help limit the spread of this superbug and contribute to a safer, healthier future.